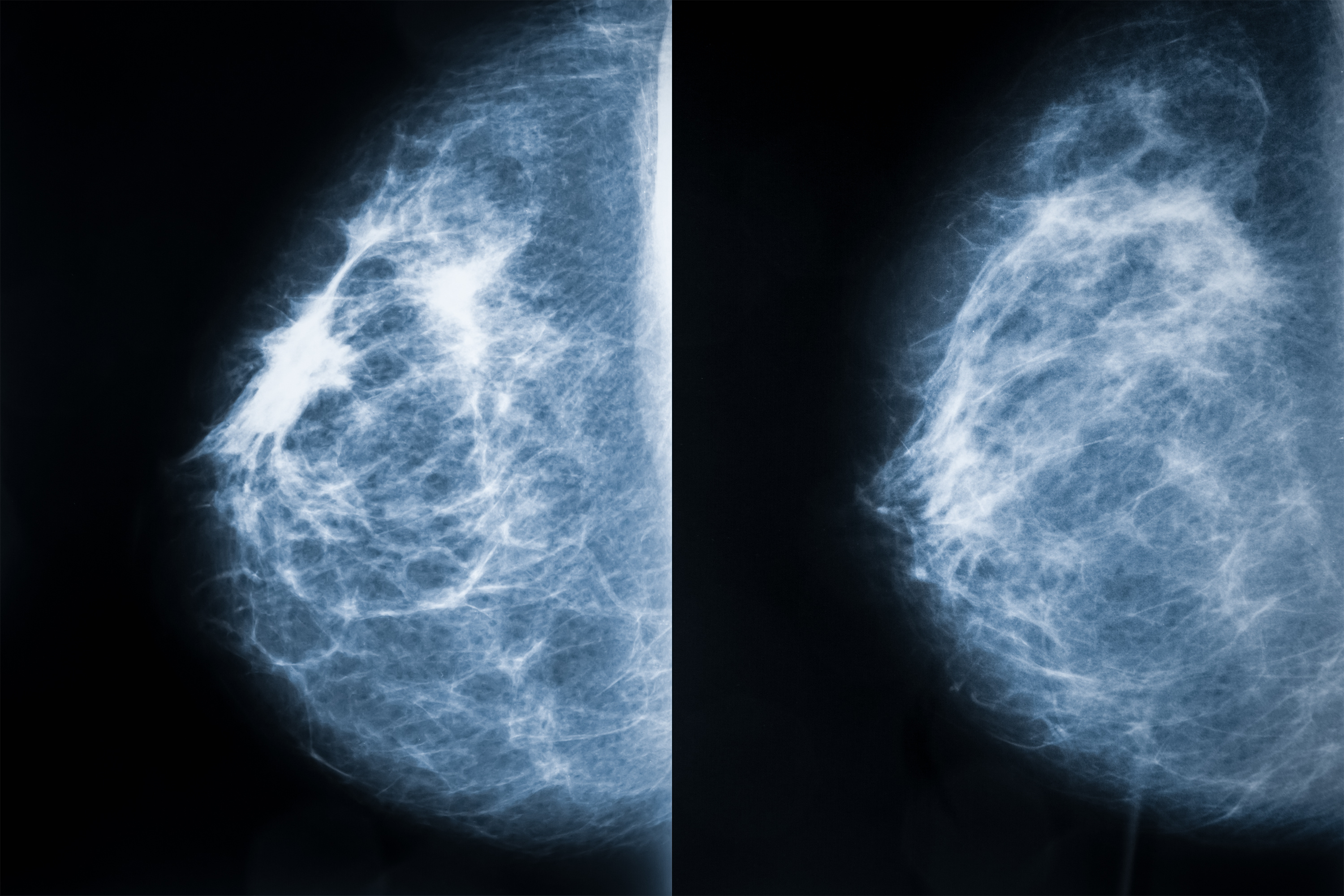
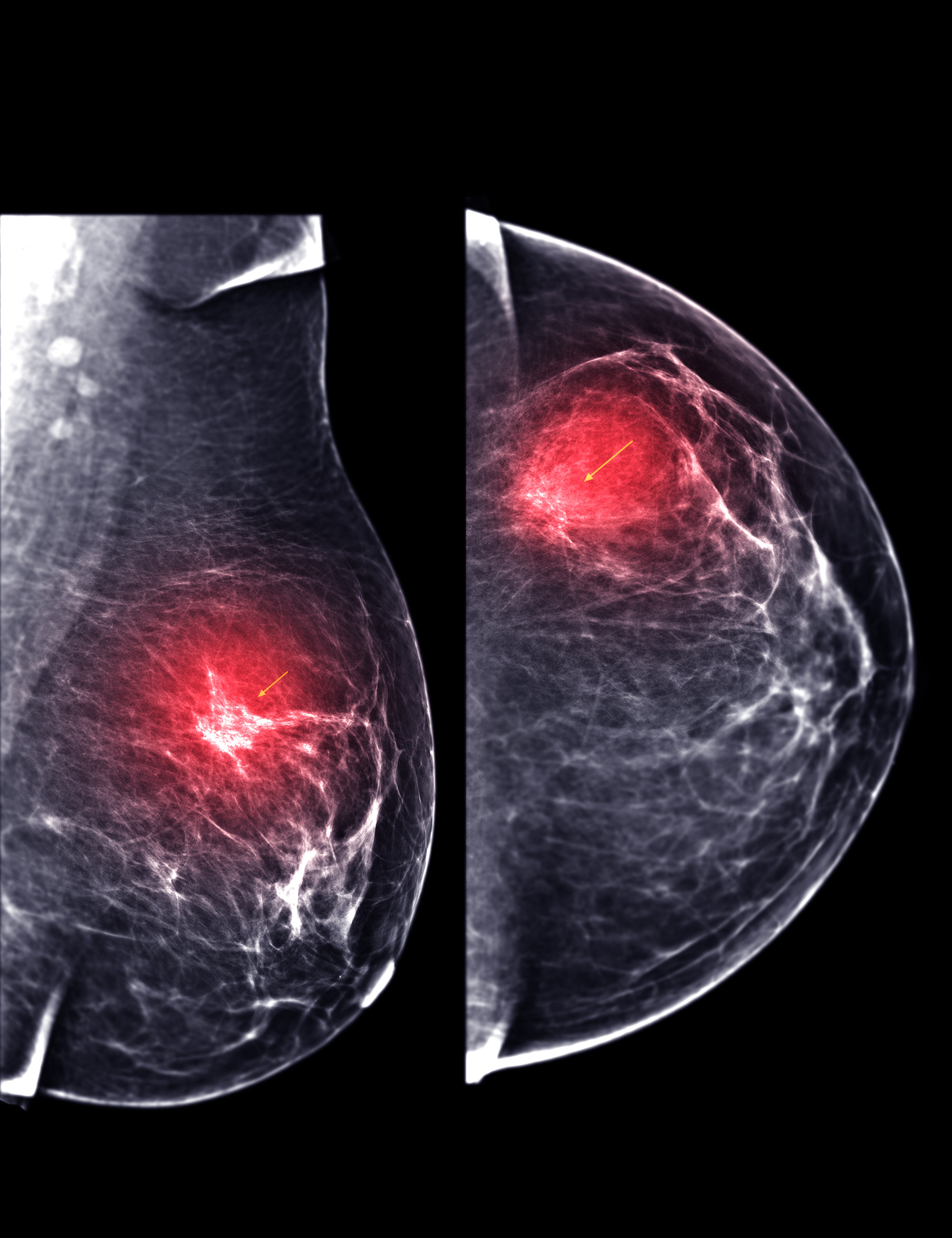
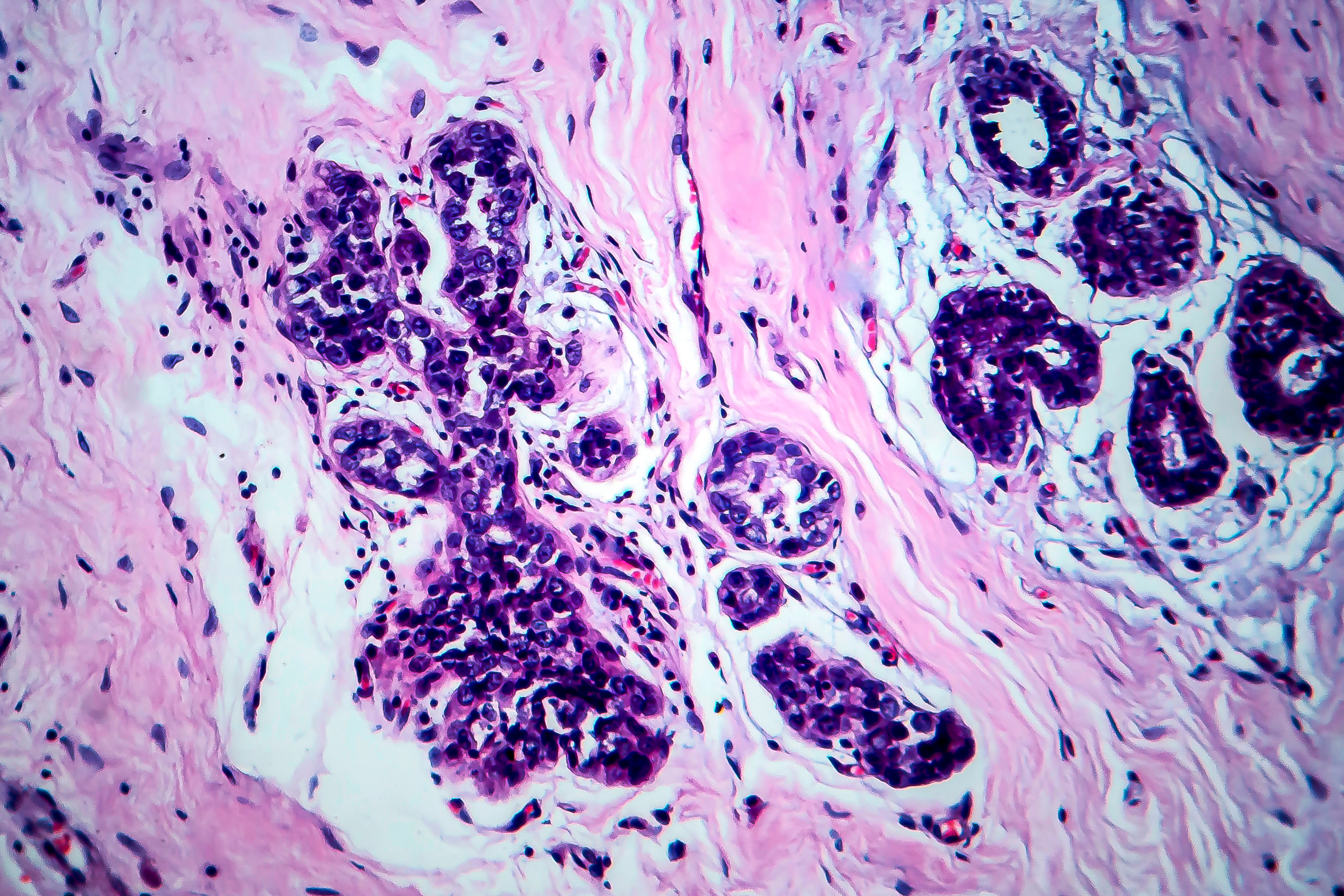
With Progesterone, the model sees tumor biology first, separating hormone-driven tumors (91.8% best-case survival) from aggressive ones (56.1% worst-case).
Without it, the model is blind to this distinction and falls back on node counts and grade alone, dropping accuracy to 64.1%.
Progesterone Status is the single most critical predictor for patient survival classification.
Regional Node Examined measures how many lymph nodes the surgeon chose to inspect, not how many had cancer. It reflects surgical procedure, not tumor biology.
Removing Regional Node Examined improves accuracy by 3.4%.